THE REALITY
Exceptions. Denials. Appeals. Caregiver follow-ups.
Your team is doing this by hand.
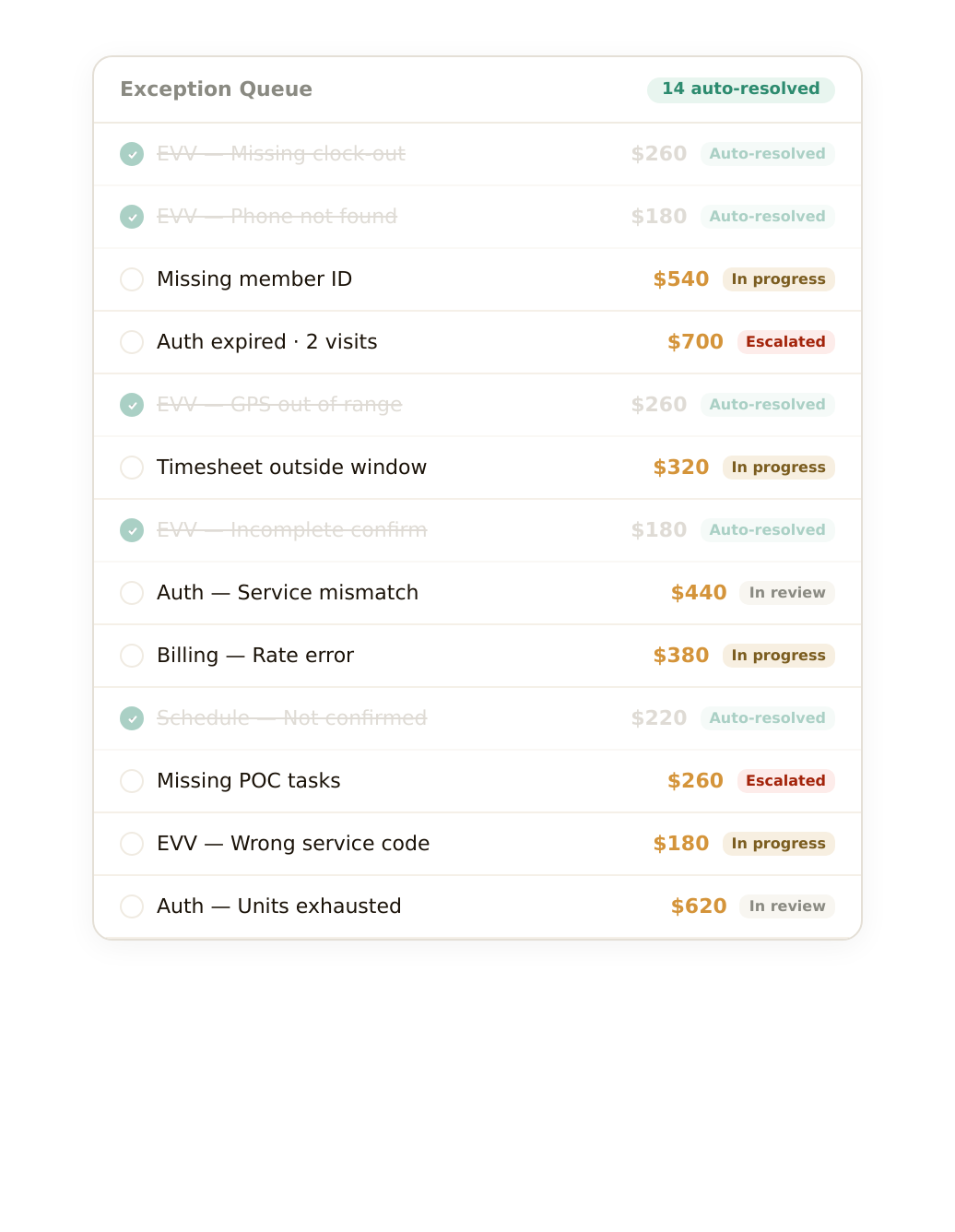
Every EVV mismatch gets investigated manually. Every denied claim gets researched, drafted, and appealed by hand. Every caregiver who didn't clock out gets a phone call. Every authorization gap gets caught — if someone has time to catch it. This is what your billing team's day actually looks like.
Meanwhile, denials age. Timely filing windows close. Recoverable revenue becomes a permanent write-off.
Your billing platform captures everything. But it doesn't tell your team what to do next. That gap between "exception flagged" and "revenue recovered" is where the money disappears.
The KELIdesk Platform
Get to know KELIdesk.
One platform for exception triage, denial recovery, caregiver outreach, and compliance. Built for home health agencies.
How It Works
Three steps to
cash flow clarity.
KELI handles the complexity so your team doesn't have to.
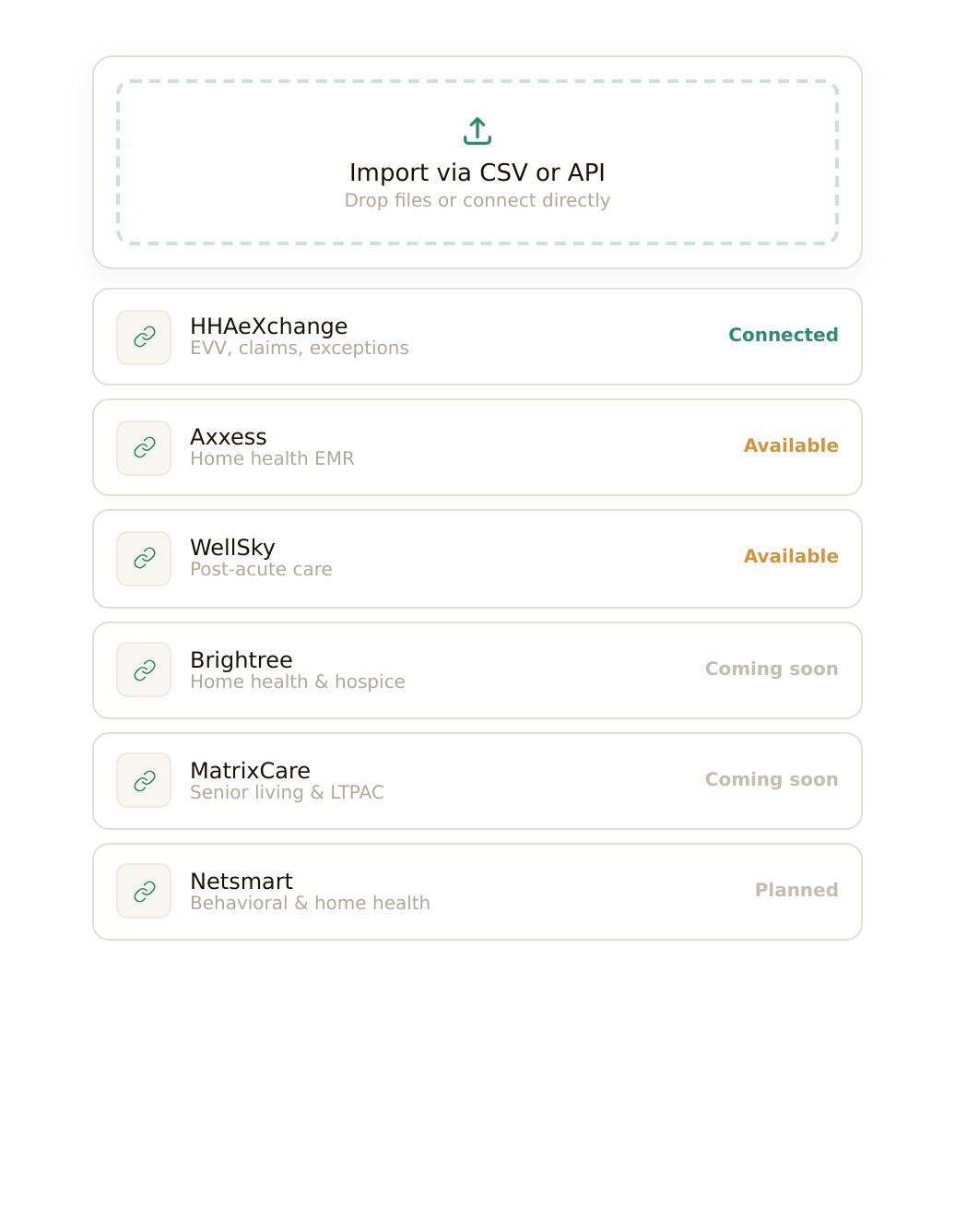
Connect.
Prioritize.
Recover.
WHAT CHANGES
When the workflow between exception and resolution is automated.
These are the outcomes KELIdesk is engineered to deliver for your agency.
30–40%
Your team submits cleaner claims
30–40% fewer first-submission denials — exceptions caught and corrected before the claim ever goes out.
<24 hrs
Your team stops chasing EVV mismatches and missing clock-outs
Routine corrections resolve automatically in under 24 hours — without anyone touching them.
85%+
Your team works the highest-value exceptions first
Every morning, automatically ranked. 85%+ of held revenue resolved within 30 days.
1 click
Your team is always audit-ready
Every action logged, timestamped, and attributed automatically. What used to take days takes one click.
Projected outcomes based on product architecture and industry benchmarks. Results vary by agency size, payer mix, and exception volume.
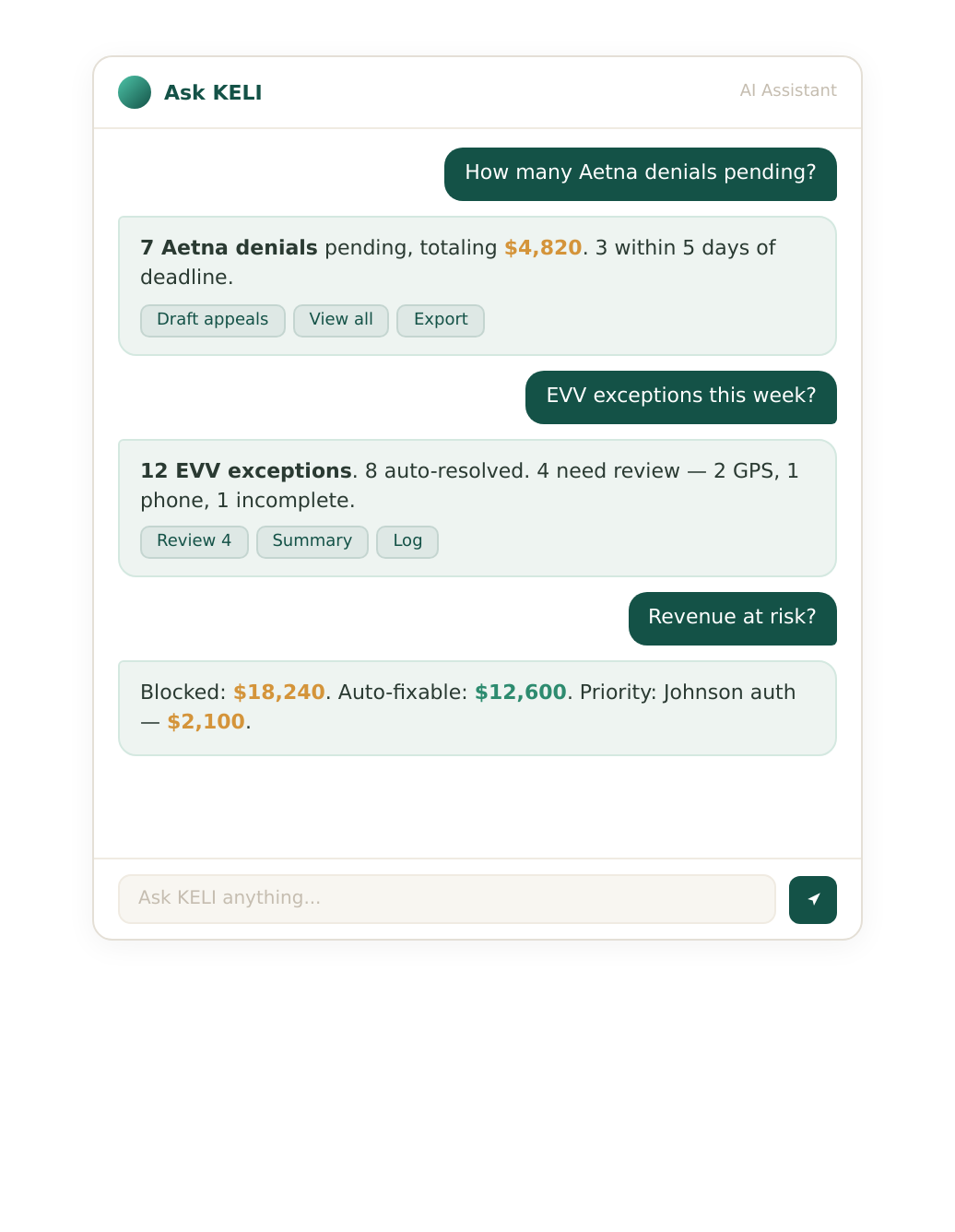
Ask KELI
Ask anything. Get answers with actions.
KELI understands your billing data. Ask a question in plain English and get instant answers backed by real numbers — plus suggested next steps you can execute immediately.
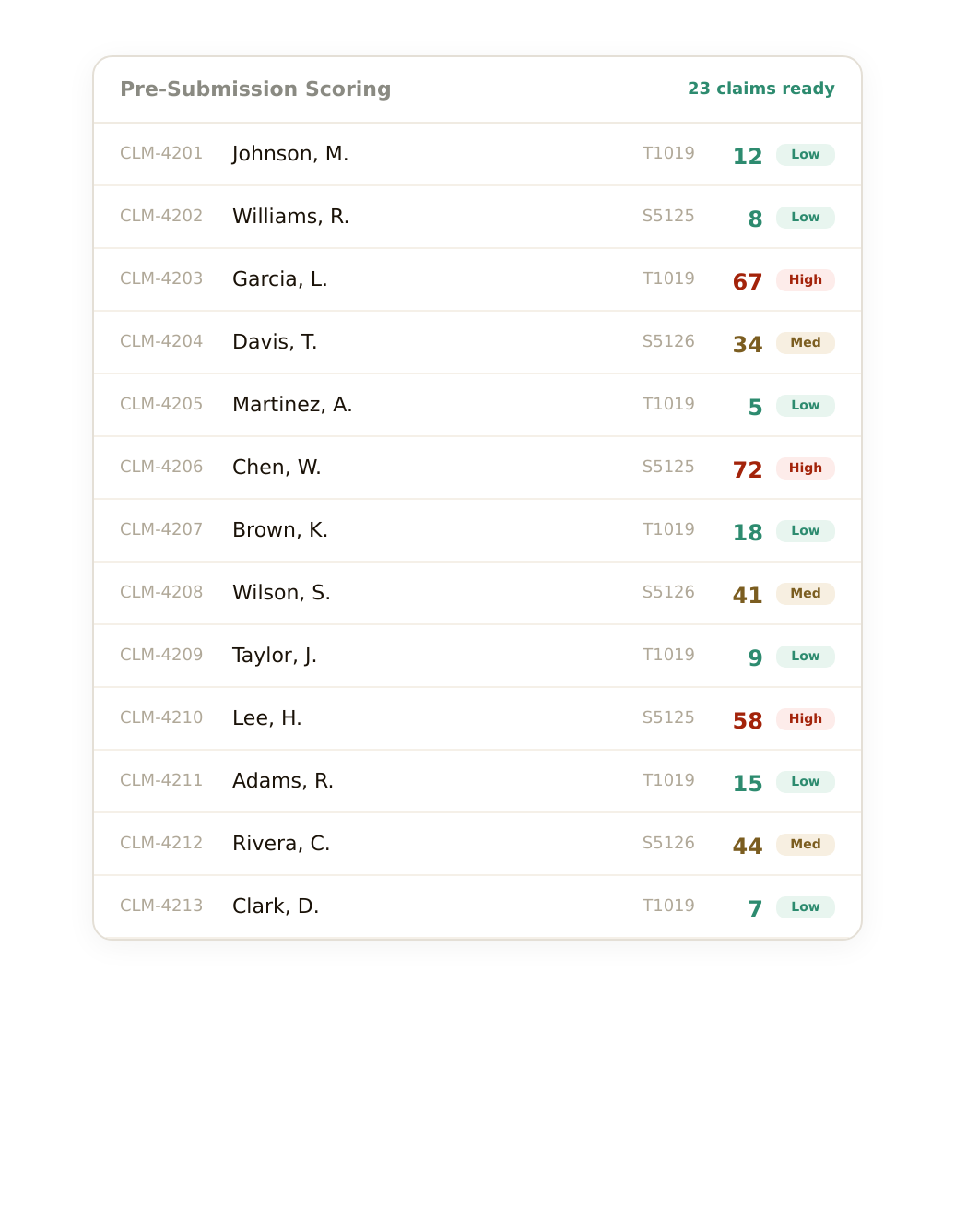
AI Triage
Every exception explained. Every fix mapped out.
When an exception lands in your queue, KELI already knows what happened, why it matters, and what to do next. No more detective work.
Caregiver Outreach
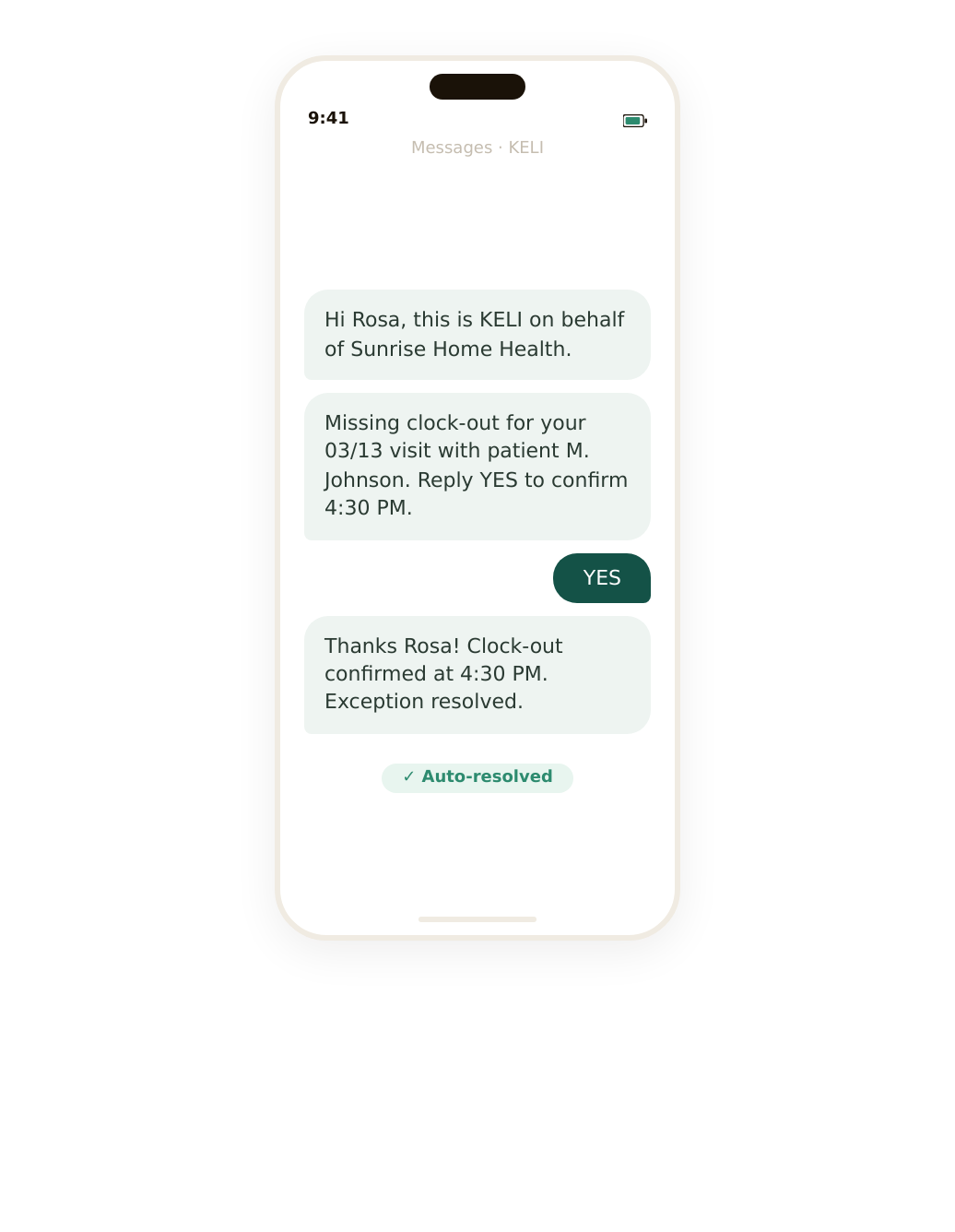
Missing EVV? KELI handles it.
When a caregiver forgets to clock out, KELI sends an SMS. No response? KELI calls. Most EVV exceptions resolve without your team lifting a finger.
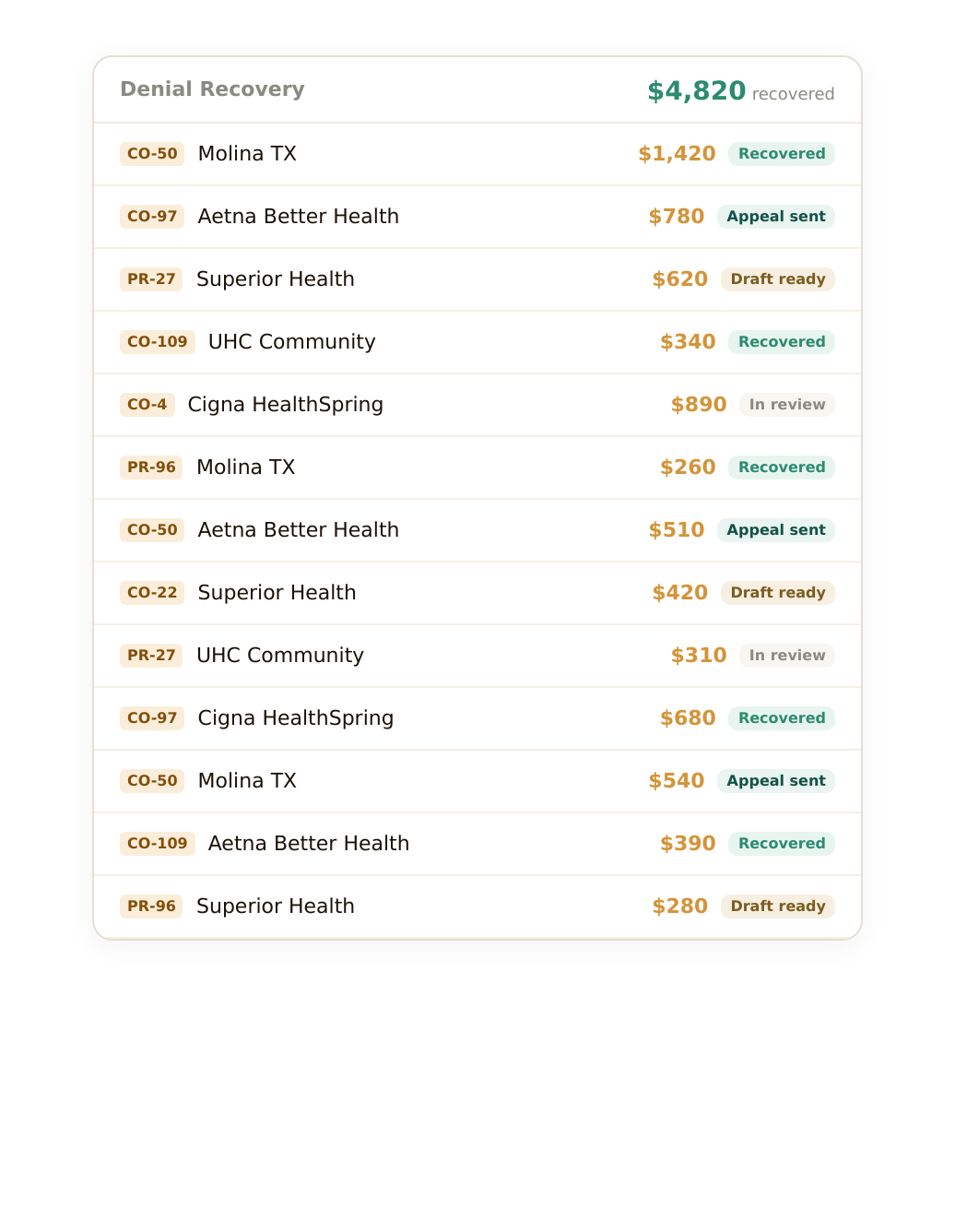
Denial Autopilot
Appeals drafted in seconds, not hours.
KELI reads the denial code, pulls your records, checks payer-specific requirements, and drafts a complete appeal letter. Your team reviews and submits.
YOUR NUMBERS
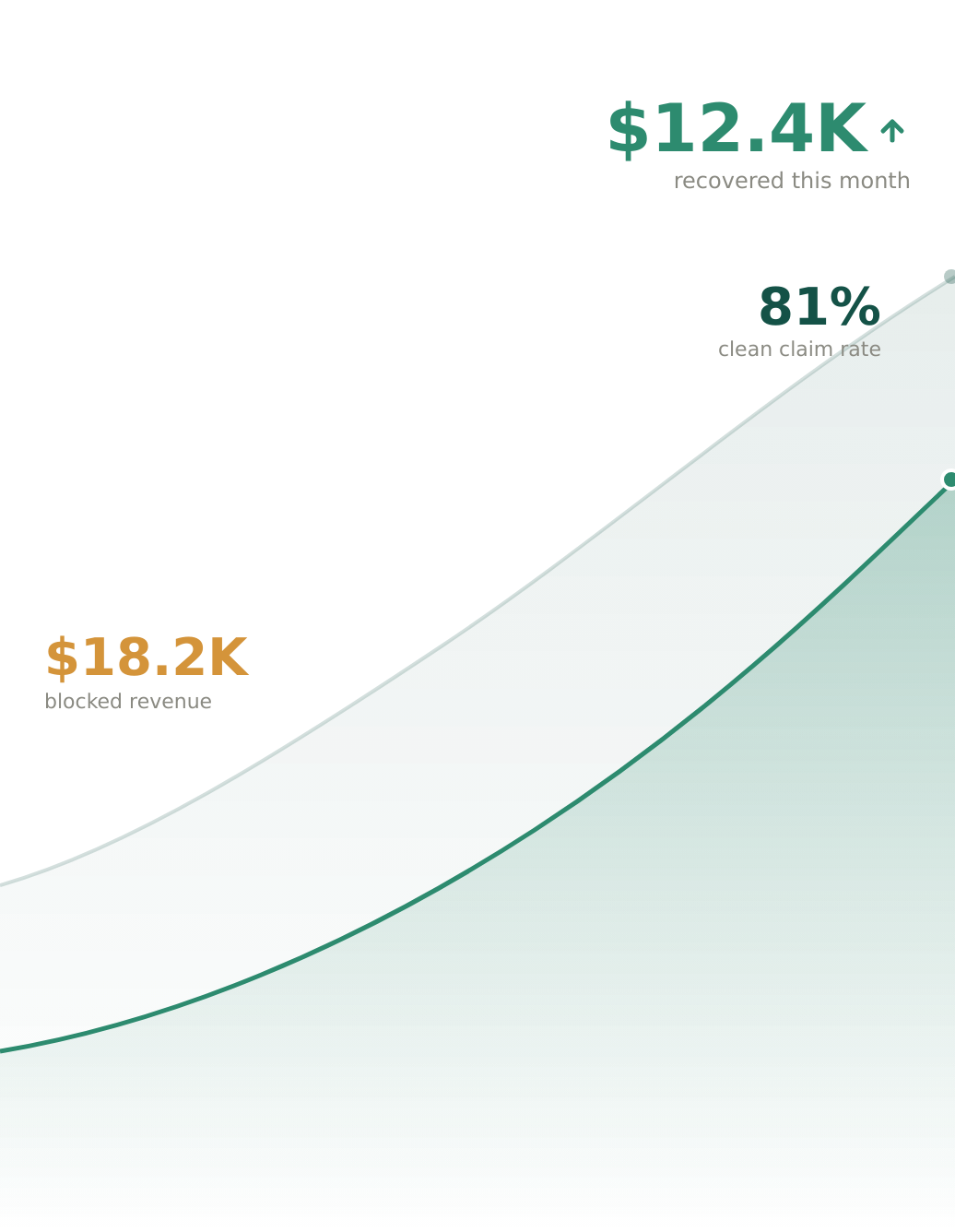
How much revenue is your agency leaving on the table?
Adjust the sliders to match your agency. Watch the math.
YOUR AGENCY
THE MATH
50% of denials are never reworked — MGMA
KELIDESK RECOVERY TARGET
Conservative 35% recovery rate. Most agencies see higher.
Based on 800 monthly claims at $220 average with 15% denial rate. Adjust sliders to match your agency. Demo uses your real data.
PRICING
Pricing that scales with your revenue.
KELIdesk protects and recovers revenue across your operation — the larger your exposure, the more system you need.
STARTER
For agencies beginning to identify revenue at risk. Foundational visibility into revenue exposure and the systems needed to stabilize operations.
Up to ~75 caregivers
GROWTH
For agencies actively managing revenue at risk. Faster recovery cycles, higher throughput, and stronger prioritization across active claims.
75–200 caregivers
ENTERPRISE
For agencies requiring maximum performance and control. Priority handling, custom workflows, and the operational depth to scale without bottlenecks.
200+ caregivers
CORE SYSTEM INCLUDED
Every plan runs on the same core system.
Scaled to your operation.
Starter
Lower volume, standard recovery pace.
Growth
Higher throughput, faster recovery cycles.
Enterprise
Maximum performance, custom workflows.
FAQ
Questions you're already asking.
And a few you haven't thought of yet.
Still have questions?